 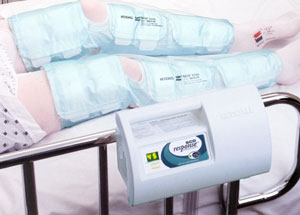
Different forms of mechanical prophylaxis alter properties in various ways such as peak venous velocity, flow rate augmentation, and duration of effect. Mechanical prophylaxis for VTE prevention comes in a variety of forms, but all are generally small variations on the same physiologic principle: increasing blood velocity decreases venous stasis and thrombosis. No two patients and/or their injury patterns are created equally, and therefore we, as the provider, must at times customize our approach to our patient’s VTE risk reduction individually. It is worth emphasizing that all modalities used in the evidence-based approach of VTE prevention should always be interpreted in the complex context of individualized patient care and not simply a comprehensive meta-analysis. With heightened attention to VTE prophylaxis, and proper application of mechanical prophylaxis devices, VTE events in the hospitalized patient can be reduced. Other unique contraindications are seen in trauma patients whose injuries prohibit placement of these mechanical prophylaxis devices due to large dressings or splints. The role of mechanical devices for prevention of VTE events is in increasing demand as pharmacologic prophylaxis is often, at least, temporarily contraindicated in trauma or critically ill patients for procedures or clinical conditions. For patients with contraindications to pharmacologic prophylaxis, and who are at risk for VTE, mechanical prophylaxis is recommended via lower-extremity compression. The current gold standard for prevention of VTE events in major trauma patients is early pharmacologic prophylaxis with the use of low dose unfractionated heparin (LDUH) or low molecular weight heparin (LMWH). 
reported deep vein thrombosis (DVT) rates as high as 58 %, and a fatal pulmonary embolism (PE) rate of 0.4 %. 
In a landmark study of trauma patients not receiving chemoprophylaxis, Geerts et al. Trauma and critically ill patients are exceedingly susceptible to VTE events as they are often prone to stasis by their immobility, have sustained endothelial injury from their trauma, and find their own immune system up regulated to a hypercoagulable state. In this review, we discuss the need for mechanical VTE prophylaxis in trauma patients, the mechanisms of clot prevention associated with the available devices, and take an evidence-based look at the efficacy of the mechanical methods available for VTE prophylaxis. Graduated compression stockings, pneumatic compression devices, foot pumps, and neuromuscular electrical stimulators are just a few of the choices in today’s providers’ armamentarium. Fortunately today, a variety of mechanical compression methods exist to assist in the optimal management of VTE prophylaxis for trauma patients. However, the potential for bleeding complications with this therapy, in a subset of major trauma patients, can have dire consequences. 
The choice of pharmacologic prophylaxis is standard for most hospitalized patients. Risk reduction of venous thromboembolic (VTE) events is paramount in the modern management of trauma patients. Trauma patients pose unique challenges when it comes to the decision for optimal thromboprophylaxis. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
